For such a small gland, the prostate causes big trouble. This year alone, 200,000 men will be diagnosed with prostate cancer. The disease kills almost as many men as breast cancer kills women.
Screening is essential
Little is known about what causes prostate cancer, although men who eat a high-fat diet seem to be at greatest risk. That’s why screening is essential.
Caught in its early stages, prostate cancer can usually be cured with surgery or radiation, and possibly helped by drug therapy. Key, of course, is catching the tumor before it spreads.
Self-defense: Once a year, starting at age 50, all men should undergo
• Digital rectal examination (DRE)
The doctor inserts a finger into the rectum to feel the prostate gland for nodules or firmness suggestive of cancer.
• Prostate-specific antigen test
This blood test measures levels of prostate-specific antigen (PSA), a protein secreted by the prostate. Elevated PSA levels suggest the need for further evaluation.
It’s important to realize that PSA levels increase with age. A level that’s normal for a man of 80, for instance, may suggest prostate cancer in a man of 45.
For men 51 or older, a level above 3.5 suggests the need for further tests. Above age 70, the cutoff is 6.5.
Getting a proper biopsy
If your PSA is high, or if the digital exam reveals a suspicious lump, it’s prudent to have the prostate biopsied.
Problem: Some doctors take just one or two tissue samples. To be sure to find any tumor (and to estimate its size), however, the doctor must take at least six tissue samples.
Other important tests
Some prostate tumors grow fast, others slowly. A slow-growing tumor might cause no trouble for years without any treatment. A virulent tumor calls for immediate, aggressive intervention.
Science has yet to find a foolproof method for telling one type of tumor from the other. However, a tumor’s Gleason score can help you pick appropriate treatment. The Gleason score is an indication of how “aggressive” the cancer cells are.
Two other tests are often helpful when making the treatment decision
• Ploidy analysis
How much DNA the tumor contains? A tumor that has either more or less DNA than normal is likely to spread.
• Polymerase chain reaction (PCR) test
This test can show whether the tumor has spread long before other tests.
Watchful waiting
If tests indicate that the tumor is small and slow-growing, treatment may be unnecessary.
As long as PSA levels stay low and the tumor grows slowly, “watchful waiting” may be appropriate. All you have to do is have a checkup every two months, including a DRE and PSA test.
Watchful waiting is generally more reasonable for a man of 70 who is likely to die of other causes before a sluggish tumor causes any trouble than a 50-year-old.
The case for surgery
If the cancer is confined to the prostate, surgical removal of the gland a procedure called radical prostatectomy is sometimes curative. Following surgery, up to 70% of men become impotent. Up to 5% become incontinent.
Innovation
Nerve-sparing prostatectomy. In this procedure, the surgeon is careful not to sever the delicate nerve bundles next to the prostate that control erection. Nerve-sparing prostatectomy is a trade-off. You’re less likely to become impotent, but there’s more risk that some cancerous tissue will remain.
What radiation has to offer
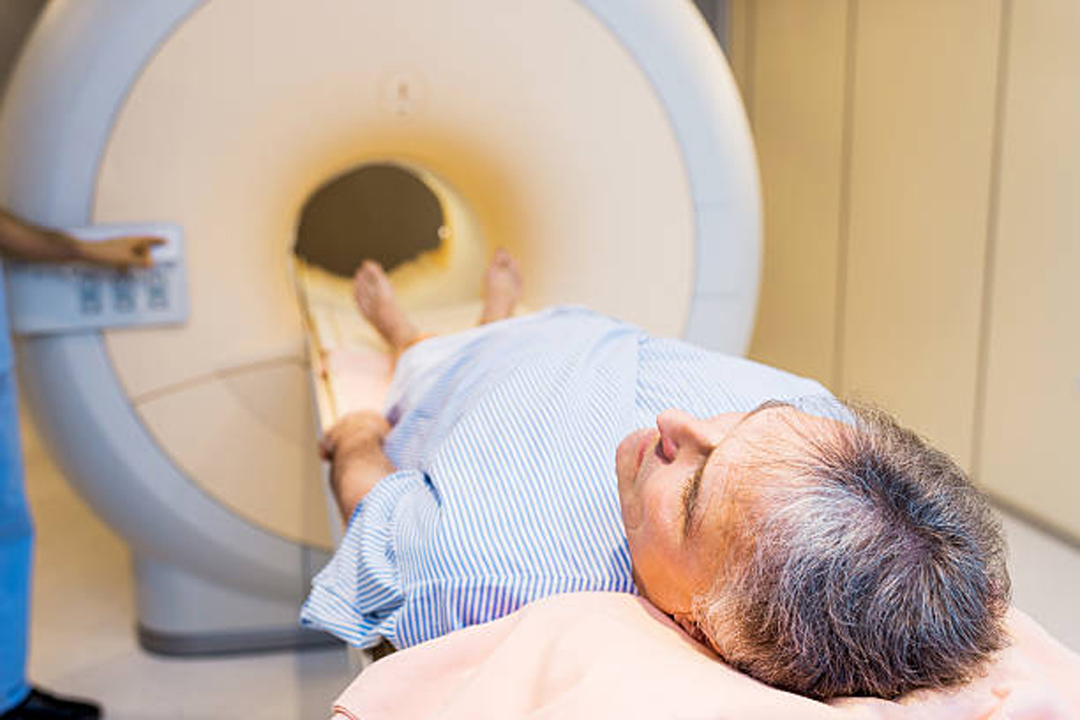
In traditional radiation therapy, a machine zaps the prostate with high-intensity X-rays.
For cancer limited to the prostate, this external beam radiation (EBR) may be as effective as surgery. Unlike prostatectomy, it doesn’t involve weeks of recovery.
Up to 50% of men who undergo radiation therapy become impotent. Incontinence is generally not a problem.
Brachytherapy is a form of radiation that is sometimes performed on an outpatient basis. In this procedure, tiny “seeds” of radioactive iodine or palladium are implanted within the prostate.
Since brachytherapy causes less damage to surrounding tissues, the impotence rate is only about 15%, the incontinence rate close to 0%. Brachytherapy delivers more radiation to the tumor.
Seed radiation seems to be just as effective as prostatectomy at curing the disease.
Hormone therapy
For prostate cancer that has spread to other tissues, prostate surgery and radiation are unlikely to extend life.
In such cases, the best strategy is to block action of testosterone and dihydrotestosterone. Secreted primarily by the testicles and adrenal glands, these male hormones spur growth of prostate cancer cells wherever they appear in the body.
Doctors can “shut down” the testicles by administering drugs called LHRH agonists or by surgically removing them in a procedure called orchiectomy.
Doctors also prescribe the drugs flutamide (Eulexin) or bicalutamide (Casodex), which block hormonal action at the cellular level. This combined hormone therapy is the treatment of choice for metastatic prostate cancer.
In a study of men with metastatic cancer, those who got combined therapy lived 1 ½ years longer than those who got single hormone therapy. Combined therapy is also used with surgery or radiation to treat cancer limited to the prostate.
Experimental approaches
In cryotherapy, the prostate is destroyed by freezing. Even with a highly skilled surgeon, this experimental therapy often causes impotence. Since it’s never been widely used, there are no long-term survival statistics.
Research suggests that modified citrus pectin, a powder derived from citrus fruit, helps stop prostate cancer from spreading.
With all the treatment options, any man with prostate cancer should consult three doctors a urologic surgeon, a medical oncologist and a radiation specialist familiar with brachytherapy.







